How Robotic Surgery Works—and Why It's Spreading
Robotic surgery uses a master-slave console system where surgeons control pencil-thin robotic arms through tiny incisions, offering greater precision and faster recovery than traditional operations.
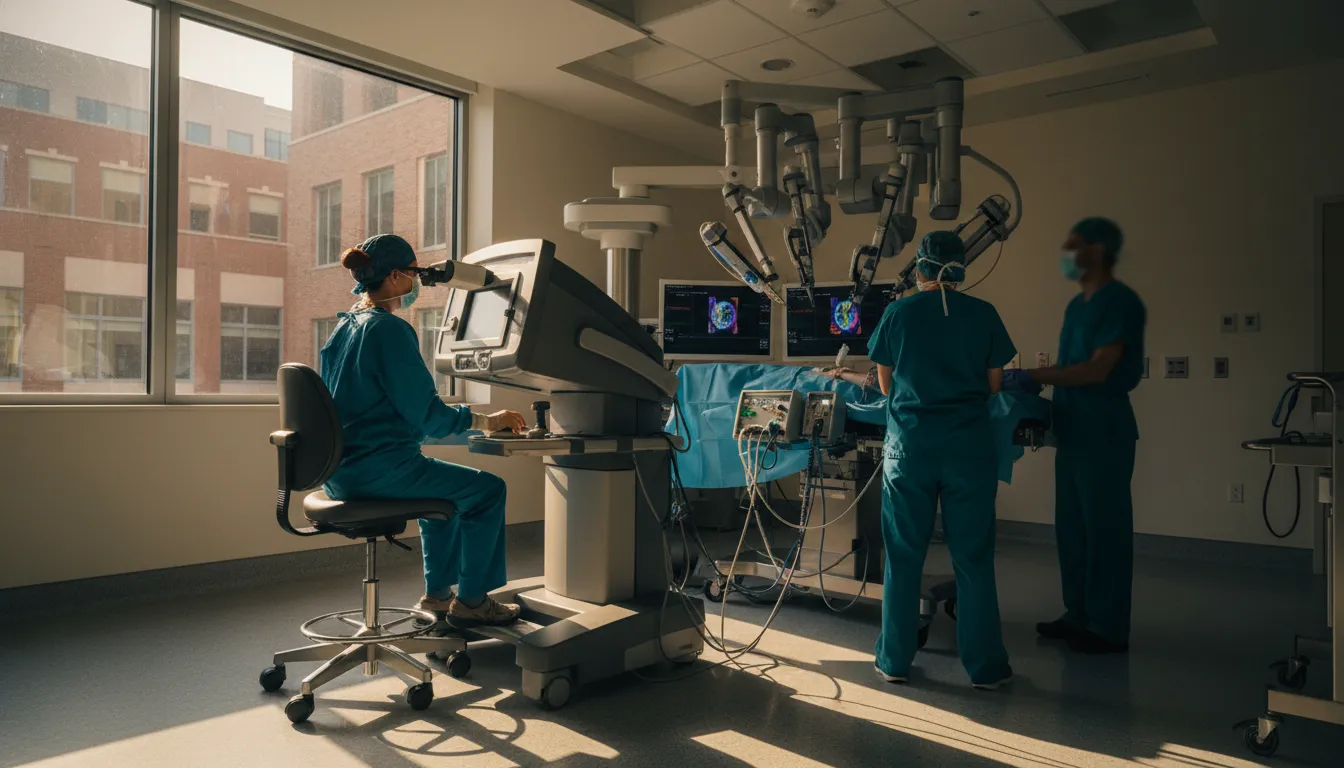
A Surgeon at a Console, Not the Table
Walk into a modern operating room and you might find the surgeon seated comfortably at a console several feet from the patient, hands inside glove-like controllers, eyes fixed on a magnified 3D display. On the operating table, four robotic arms—each thinner than a pencil—reach through incisions barely a centimetre long. This is robotic-assisted surgery, one of the fastest-growing fields in modern medicine.
Despite the name, no robot operates autonomously. Every movement of the instruments follows the surgeon's hands in real time. The machine is a tool—an extraordinarily precise one—but the human remains firmly in charge.
How the System Works
The dominant platform, Intuitive Surgical's da Vinci system, consists of three core components: a surgeon's console, a patient-side cart with robotic arms, and a video tower that processes and displays imagery.
At the console, the surgeon views a high-definition 3D image magnified up to ten times beyond what the naked eye can see. Hand controllers translate finger and wrist movements into micro-scale actions at the instrument tips. A built-in computer filters out the surgeon's natural hand tremor, delivering smoother motion than any human hand could achieve unaided.
The robotic arms grip interchangeable instruments—scalpels, scissors, graspers, electrocautery tools—each with seven degrees of freedom, exceeding the range of a human wrist. This lets surgeons reach angles and spaces that conventional laparoscopic tools cannot. One arm always carries a camera, providing the 3D feed that guides the procedure.
Why Surgeons and Hospitals Adopt It
The core appeal is minimally invasive precision. Traditional open surgery requires large incisions, long recovery, and significant blood loss. Conventional laparoscopy shrinks the incisions but limits the surgeon's dexterity. Robotic assistance bridges the gap: small incisions with full range of motion.
Studies consistently show that robotic procedures reduce postoperative pain, shorten hospital stays, lower complication rates, and speed recovery. A 2026 University of Hong Kong study found that robotic-assisted total hip replacements significantly reduced the need for repeat operations compared with traditional methods.
For surgeons, the ergonomic benefits are substantial. Operating from a seated position reduces the physical fatigue that can degrade performance during procedures lasting many hours.
The Numbers Behind the Growth
Since the FDA first approved robotic surgical assistance in 2000, adoption has accelerated sharply. Over 10 million robotic procedures have been performed worldwide using da Vinci systems alone, with more than 6,700 units installed across 69 countries. Robotic surgeries now account for roughly 15% of all surgical procedures globally.
The market reflects this momentum. Valued at approximately $12 billion in 2024, the global surgical robotics market is projected to reach $27–42 billion by the early 2030s, according to multiple industry analyses, with annual growth rates between 15% and 18%.
Risks and Limitations
Robotic surgery is not without concerns. An analysis of 14 years of FDA adverse-event data found over 10,600 reports, including 144 deaths and nearly 1,400 patient injuries. Device malfunctions—broken instrument fragments falling into patients, electrical arcing, and system errors—accounted for the majority of reports.
The learning curve is steep. Estimates for achieving proficiency range from 40 to 250 cases depending on the procedure, and robotic operations typically take about 30 minutes longer than their traditional equivalents.
Cost remains a major barrier. A single da Vinci system costs $1.5 to $2 million, with ongoing expenses for maintenance, instrument replacement, and surgeon training. In 2019, the FDA warned that long-term survival benefits of robotic cancer surgeries had not yet been established, urging caution in certain oncological applications.
What Comes Next
New competitors are entering the market with systems designed to lower costs and expand capabilities. Advances in haptic feedback—allowing surgeons to "feel" tissue resistance through the controllers—aim to close the sensory gap between robotic and direct-contact surgery. Meanwhile, AI-assisted guidance systems are being developed to help identify anatomical structures in real time, potentially reducing errors and shortening training periods.
Robotic surgery will not replace surgeons. But as systems grow cheaper, smarter, and more widespread, the line between what a human hand can do and what technology can enhance continues to shift—overwhelmingly in the patient's favour.


