How Telesurgery Works: Operating From Miles Away
Telesurgery lets surgeons operate on patients thousands of miles away using robotic arms and fiber-optic connections. Here's the science and technology behind it.
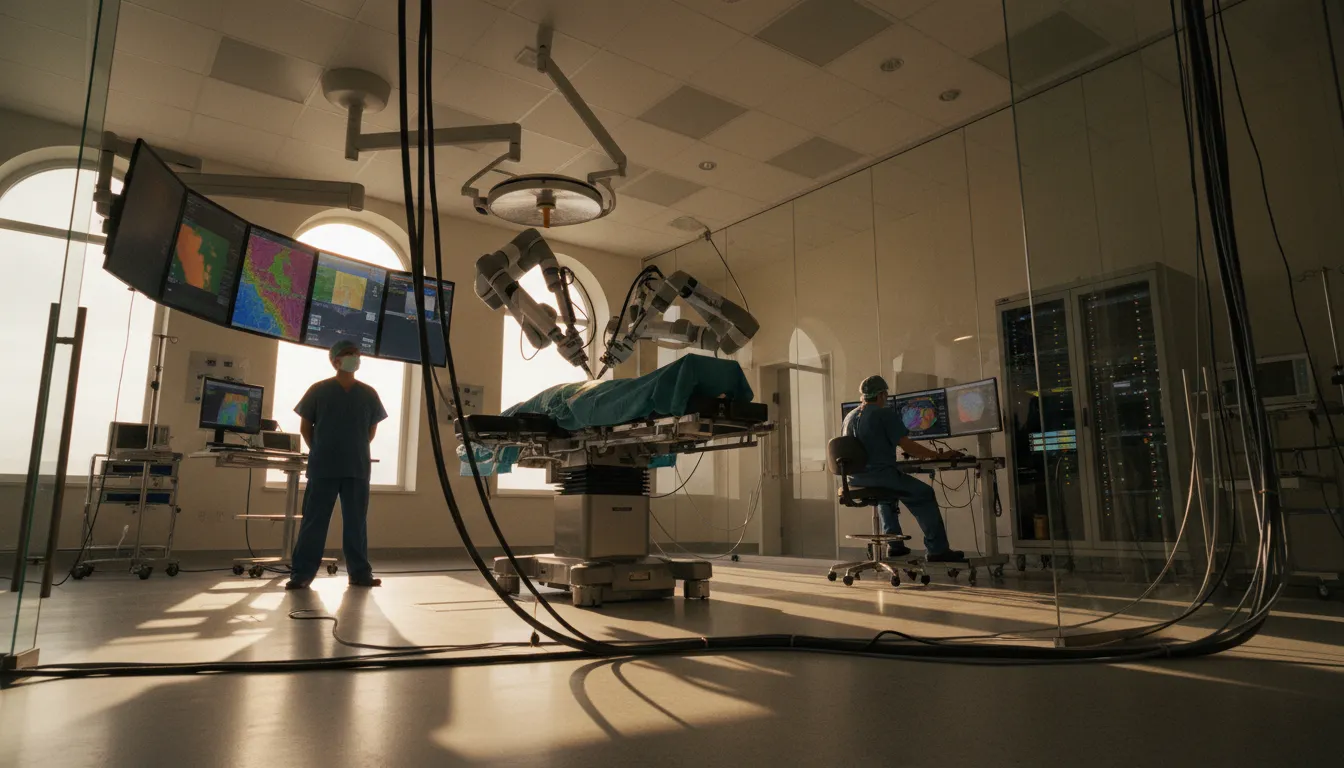
A Surgeon in London, a Patient in Gibraltar
A 62-year-old man lies on an operating table in Gibraltar. His surgeon is 1,500 miles away in London, seated at a console in a Harley Street clinic. Four robotic arms inside the Gibraltar hospital mirror the surgeon's hand movements within 60 milliseconds — faster than a human eye-blink. The result: a successful cancer operation that neither patient nor surgeon could tell apart from a conventional one.
This is telesurgery — remote robotic surgery — and it is rapidly moving from science fiction to clinical reality. But how, exactly, does it work?
The Basic Architecture
Every telesurgical system has three core components: a surgeon's console, a communication network, and a robotic unit at the patient's bedside.
The surgeon sits at a master console equipped with hand controllers, foot pedals, and a high-definition 3D display. Every movement of the surgeon's hands — including tremor-filtered micro-movements — is digitized and transmitted over a network to the robotic unit. That unit converts the signals back into precise mechanical movements of surgical instruments inside the patient's body. Video and sensor data flow back to the surgeon in near-real time, giving them a view of the operative field comparable to open surgery.
Modern systems like the Toumai robot (used in the London–Gibraltar case) and the da Vinci platform also filter out involuntary hand tremors, making robotic incisions more stable than those of an unaided human hand.
Why Latency Is Everything
The most critical technical challenge in telesurgery is latency — the delay between a surgeon's movement and the robot's response. According to peer-reviewed research published in PMC, surgeons can compensate for delays up to about 200 milliseconds without significant skill loss. At 300 ms, performance begins to degrade noticeably. Above 700 ms, telesurgery becomes unsafe.
This is why network technology matters so much. Early systems relied on dedicated fiber-optic lines. The landmark Lindbergh Operation of September 2001 — when Professor Jacques Marescaux removed a patient's gallbladder in Strasbourg while operating from New York, a distance of over 14,000 kilometres — achieved a latency of 135 ms using a high-speed transatlantic fiber link. It was the world's first transcontinental telesurgical operation.
How 5G Is Changing the Equation
For decades, telesurgery depended on expensive, fixed fiber-optic infrastructure. The rollout of 5G wireless networks is transforming what is possible. According to Ericsson, 5G's Ultra-Reliable Low-Latency Communications (uRLLC) mode can achieve user-plane latencies as low as 0.5 milliseconds — far below what any surgical procedure requires.
In practice, real-world 5G telesurgery latencies hover between 20 and 130 milliseconds depending on distance and network conditions. Hybrid setups — fiber as the primary link, 5G as an automatic backup — are becoming the standard. The London–Gibraltar surgery used exactly this architecture: fiber-optic cable as the main channel, with a 5G backup ensuring continuity if the primary link failed.
What Happens During the Surgery
The workflow of a telesurgical procedure closely mirrors a conventional robotic operation:
- A local surgical team prepares the patient and positions the robotic unit.
- The remote surgeon reviews imaging and connects to the robotic console.
- The network link is tested and latency verified before the first incision.
- The surgeon operates using the console; local staff monitor and can intervene if needed.
- Video, audio, and haptic (touch) feedback stream back to the surgeon continuously.
Haptic feedback — the sense of resistance and texture — remains an active research area. Current systems offer limited tactile sensation, meaning surgeons rely heavily on visual cues. Next-generation platforms aim to restore fuller haptic feedback over 5G and eventually 6G connections.
Why It Matters for Global Healthcare
The most transformative application of telesurgery is not convenience — it is access. Billions of people live in regions with few or no specialist surgeons. A rural hospital in sub-Saharan Africa or a military field station could, in principle, access world-class surgical expertise through a robotic unit and a satellite or 5G link.
Milestones keep falling. In July 2025, a bariatric surgeon in Strasbourg operated on a patient in Indore, India — 8,500 kilometres apart — without perceptible lag. Teams at the University of Florida have performed procedures from Orlando to Dubai, covering 12,400 kilometres. Each success narrows the gap between where the best surgeons are and where patients actually need them.
The Road Ahead
Regulatory frameworks, liability questions, and the cost of robotic hardware remain significant barriers to widespread adoption. Training surgeons to operate without physical presence — and to trust a network link with a patient's life — requires new protocols and rigorous credentialing.
But the technology itself has already proven its case. From the Lindbergh Operation's 135-millisecond transatlantic leap in 2001 to a 60-millisecond London-to-Gibraltar prostatectomy decades later, telesurgery has crossed a threshold from research curiosity to genuine clinical tool. The question is no longer whether remote surgery works — it is how quickly the world can build the infrastructure to make it routine.


